Bowel resection should be indicated restrictively. An aggressive approach for endoscopic removal is justified because the frequency of tumors decreases as the patients become older ( Goodman 1998). The small intestinal polyps may be resected during laparotomy by means of endoscopes or enterotomy. This because the focus organs of the polyps concerning frequency are the duodenum and the small intestine. Solitary Peutz-Jeghers’ polyps in the colon may be resected by colonoscopy. 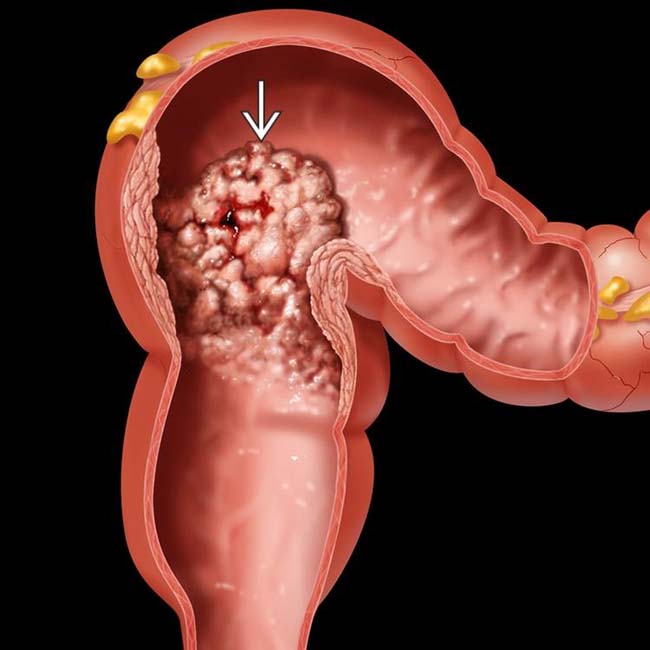
The histological work-up suggests a lesion representing a hamartomatous process or malformation rather than a neoplasm ( Morson 1962). Contrast studies and endoscopy show the extend of the disease. Rectal bleeding is another frequent symptom. The most common signs are abdominal pain often due to intestinal obstruction (polyps themselves or an intussusception). Diagnosis of the syndrome is based on family history, skin pigmentation and gastrointestinal symptoms. In 100% these polyps occur in the small bowel (colon 30%, stomach 25%) ( Crawford 1994). They tend to be large and pedunculated, histologically, it’s an network of connective tissue and well developed smooth muscle extending into the polyp. Multiple polyps scattered throughout – the entire gastrointestinal tract and melanotic mucosal and cutaneous pigmentation around the lips, oral mucosa, face, genitalia and palmar surfaces of the hands (Robbins 1994). Peutz-Jeghers’ polyps occur singly or multiple in the Peutz-Jeghers’ syndrome which is a rare autosomal dominant disease. An index person indicates colorectal evaluation of the family members. Because of the ileal reservoir neoplasms a follow-up of periodic endoscopy together with the upper gastrointestinal tract should be initiated. If there are too many polyps, restorative proctocolectomy with ileal pouch should be considered. All juvenile polyps should be resected by means of colonoscopy. In most cases this disease is identified in childhood.Īs juvenile polyposis is considered a potential premalignant condition an aggressive management is indicated ( Longo 1990). The appearance of the disease is associated with benign and malignant neoplasms of the gastrointestinal tract. A fatal form of juvenile polyposis in infancy is characterized with profuse diarrhea, protein losing enteropathy, bleeding and rectal prolapse ( Desai 1995). There are extracolonic congenital and acquired manifestations as macrocephaly, alopecia, bony swellings, cleft lip, cleft palate, double renal pelvis and ureter, acute glomeronephritis undescended testicle and bifid uterus and vagina ( Desai 1995). Symptoms and signs are hematochezia, iron deficiency anemia, hypoproteinemia, hypokalemia, anergy ( Grosfield 1986). The recurrence rate of solitary juvenile polyps is < 20% whereas the rate in familial cases is nearly 90% ( Haggitt 1970). There is a family history in about 20 to 50% of patients ( Rickert 1979). Juvenile polyposis syndrome is an uncommon condition in which multiple juvenile polyps arise in the colon but also in the intestinal tract. Once the single polyp is removed no further follow-up is required. A juvenile polyp is neither a neoplasm nor a premalignant condition. In case of a juvenile polyp the whole colon should be explored (cp. The section surface shows a cystic appearance with spaces filled with mucous.ĭiagnosis is confirmed by histology of the endoscopically resected polyp. The majority of these polyps are larger than 1 cm in diameter. Nearly 80% occur in the rectum but they may be scattered throughout the colon ( Mazier 1982, Jalihal 1992). It is the most frequent colorectal tumor in children. The incidence in boys (men) is higher ( Roth, 1963) than in girls (women). Juvenile polyp (congenital polyp, retention polyp, juvenile adenoma) usually occurs in children under ten years of age ( Morson 1962).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
